Fracking Activities May Contribute to Anxiety and Depression During Pregnancy by Columbia University’s Mailman School of Public Health, July 24, 2019, Science Daily
A new study identifies a link between proximity to hydraulic fracking activities and mental health issues during pregnancy.
A new study led by a researcher at Columbia University Mailman School of Public Health identifies a link between proximity to hydraulic fracking activities and mental health issues during pregnancy. Results appear in the journal Environmental Research.
The researchers looked at 7,715 mothers without anxiety or depression at the time of conception, who delivered at the Geisinger Health System in Pennsylvania between January 2009 and January 2013. They compared women who developed anxiety or depression during pregnancy with those who did not to see if the women’s proximity to hydraulic fracturing activity played a role. Hydrofracking locations were available through public sources.
They found that for every 100 women, 4.3 additional women would experience anxiety or depression if they lived in the highest quartile of exposure compared to the other quartiles. The prevalence of anxiety or depression during pregnancy was 15 percent in the highest quartile, compared to just 11 percent in the lower three quartiles. The risk appeared greater among mothers receiving medical assistance (an indicator of low income) compared to those who did not: the authors observed 5.6 additional cases of anxiety or depression per 100 exposed women. They found no relationship between anxiety or depression during pregnancy and preterm birth and reduced term birth weight (an earlier study the research team found a link between proximity to hydrofracking and these adverse birth outcomes).
First author Joan Casey, PhD, assistant professor in the Department of Environmental Health Sciences, points to several possible reasons why living near fracking sites could lead to mental health problems in women. “Fracking activities may act as community-level stressors by degrading the quality of the natural environment, neighborhoods, such as by the production of toxic wastewater and increases in truck traffic, leading residents to feel a lack of control that harms their health,” says Casey. “Another possibility is that air pollution from the sites could be directly contributing to mental health problems in this vulnerable population. Future research could examine other potential factors like air quality, noise, light pollution, psychosocial stress, and perception of activities.”
Story Source:
Materials provided by Columbia University’s Mailman School of Public Health.
Unconventional natural gas development and adverse birth outcomes in Pennsylvania: The potential mediating role of antenatal anxiety and depression by Joan A.Casey, Dana E. Goin, Kara E. Rudolph, Brian S. Schwartz, Dione Mercer, Holly Elser, Ellen A. Eisen, Rachel Morello-Frosch
Highlights
• Unconventional natural gas development has been linked to adverse birth outcomes.
• No studies have considered the role of antenatal mental health.
• Unconventional natural gas development was associated with antenatal anxiety or depression.
• This association did not mediate the original exposure-birth outcome relationship.
Abstract
Background
Studies have reported associations between unconventional natural gas development (UNGD) and adverse birth outcomes. None have evaluated potential mediating mechanisms.
Objectives
To evaluate associations between (1) UNGD and antenatal anxiety and depression and (2) antenatal anxiety and depression and preterm birth (<37 weeks gestation) and reduced term birth weight, (3) stochastic direct and indirect effects of UNGD on preterm birth and term birth weight operating through antenatal anxiety and depression, and (4) effect modification by family-level socioeconomic status.
Methods
This retrospective cohort study included mothers without prevalent anxiety or depression at time of conception, who delivered at Geisinger in Pennsylvania between January 2009–January 2013. We assembled phase-specific UNGD activity data from public sources. Mothers were categorized as exposed (quartile 4) or unexposed (quartiles 1–3) based on average daily inverse distance-squared UNGD activity metric between conception and the week prior to anxiety or depression (cases) or the pregnancy-average daily metric (non-cases). We estimated associations with a doubly robust estimator (targeted minimum loss-based estimation) and adjusted for potential individual- and community-level confounding variables.
Results
Analyses included 8,371 births to 7,715 mothers, 12.2% of whom had antenatal anxiety or depression. We found 4.3 additional cases of antenatal anxiety or depression per 100 women (95% CI: 1.5, 7.0) under the scenario where all mothers lived in the highest quartile of UNGD activity versus quartiles 1–3. The risk difference appeared larger among mothers receiving Medical Assistance (indicator of low family income) compared to those who did not, 5.6 (95% CI: 0.5, 10.6) versus 2.9 (95% CI: -0.7, 6.5) additional cases of antenatal anxiety or depression per 100 women. We found no relationship between antenatal anxiety or depression and adverse birth outcomes and no mediation effect either overall or when stratifying by Medical Assistance.
Conclusion
We observed a relationship between UNGD activity and antenatal anxiety and depression, which did not mediate the overall association between UNGD activity and adverse birth outcomes.
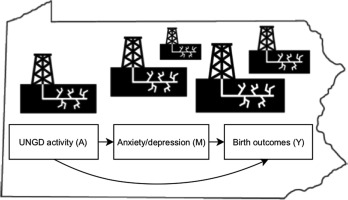
Graphical abstract